Photo: Jane Teeling
By Taylor Tepper and Jacob Hodes
Published: May 22, 2012
In the jargon of the medical world, doctors practice “primary care” or they “specialize.” The specialists take care of things like your brain, heart, intestinal tract and feet. The primary-care physicians are your family doctors. They take care of everything.
In New York City, we are told that primary care is in crisis. That is what we set out to explore in this series of articles, and we discovered that we were told right. New York’s primary-care doctors do not cover enough of the city now, and unless trends change, they will cover even less of the five boroughs in the future.
As a whole, the city has plenty of doctors. But when it comes to primary care, there are two New Yorks: the forest and the desert. If you live in the Upper East Side, Chelsea or Soho, you live in the forest. Northern Bronx? East New York? South Jamaica? You live in the desert.
The city needs more primary-care doctors. But fewer young doctors are choosing to practice primary care in the city, and this means that the healthcare deserts will likely expand.
A minimum of 50 primary-care doctors – defined as family-care physicians, pediatricians and general internists – are needed for every 100,000 residents, according to guidelines established by the Department of Health and Human Services. In New York City, there are 261 doctors for every 100,000 residents on the Upper East Side, but only 34 in the northeast Bronx.
In the city as a whole, 1.1 million adults – or 18 percent of the adult population – have no regular primary-care provider, according to a recent city study.
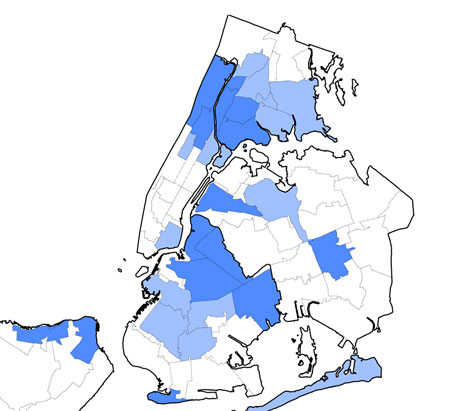
Large swaths of New York City are classified as Health Professional Shortage Areas by the U.S. Department of Health and Human Services. Click the map for a more detailed view.
By 2030, the city will be short several thousand additional primary-care providers, according to a recent study by the Center for Health Workforce Studies at SUNY Albany’s School of Public Health. (Its researchers predict the additional shortage will fall between 1,200 and 3,200 doctors, depending on factors such as economic growth, future healthcare reforms and consumer behavior.)
“If we don’t do something, we’re going to have a really big problem,” said Gaetano Forte, a researcher at the center and an author of the study.
It won’t be easy to turn that trend around, because as older doctors retire, fewer young doctors are choosing to practice primary care in the city. These young doctors know that they will make much more money if they specialize.
If recent medical school graduates do choose to practice primary care, they are more likely to do so in wealthy communities, where patients can either pay more or have more generous insurance policies. Others are leaving New York or finding jobs as internists at hospitals, rather than practicing in the community-based clinics where they are needed most.
This is not to say that young doctors are selfish: they have to earn a lot of money, since the average loan debt taken on by med school students is now $140,000, an increase of $50,000 since 1994.
So here is the healthcare environment facing the city within the next couple of decades: a shrinking forest lush with world-class primary care, and an expanding desert of poor and not-so-poor people who can expect haphazard care and long lines at the clinic or emergency room.
The crucible
With vast disparities in income and access to insurance, New York is a perfect crucible for healthcare problems. In our series of stories, you will read that ambulances are overused and emergency rooms are overcrowded. Women all over the city find it difficult to obtain affordable birth control by prescription. And health clinics are overburdened.
More than 900,000 people in Brooklyn – more than a third of the borough’s population – live within federally designated Health Professional Shortage Areas. The ratio is similar in the Bronx.
The community-based clinics that serve these areas, where a majority of the city’s more than 3 million Medicaid patients live, cannot meet demand. So, in the city’s desertlands, New Yorkers without access to primary care are using ambulances and emergency rooms for routine medical needs.
More than 900,000 people in Brooklyn – more than a third of the borough’s population – live within federally designated Health Professional Shortage Areas. The ratio is similar in the Bronx.
In 2011, the city’s 911-dispatched emergency services responded to more than 1.2 million calls citywide. Of these, nearly three in four were not life threatening. “We’re a taxi half the time,” EMT Stephen Katz told us. By law, the ambulances cannot turn patients away.
In the city’s emergency rooms, staff members talk about “frequent fliers” — patients who show up often for minor problems. “You see a lot of people coming here who don’t necessarily need to,” said Kimberly Gordon, 29, a nurse practitioner at Lenox Hill Hospital’s emergency department. “It’s a problem, but it only seems to be getting worse because we have no choice but to treat them.”
The need for more primary-care doctors is clear, and demand may grow. The Affordable Care Act, or Obamacare, provides funding for several new primary-care initiatives. And by bringing previously uninsured patients into the system, it may exacerbate the doctor shortage. (The Supreme Court will rule on the act’s constitutionality in June.)
Nonetheless, in medical schools students are voting with their feet for other specialties. Healthcare leaders in the field complain that most of the country’s major medical schools steer students elsewhere. From 1998 to 2008, the number of family medicine residencies declined by 400, while those for such specialists as cardiologists and oncologists increased by 1,150.
“There’s every reason not to practice primary care,” said Greg Katz, a recent graduate of New York University’s medical school who is still wrestling with his career decisions. He ticked off the problems: other specialties provide more prestige, better working conditions, and higher pay. Specialists make $400,000 or more, according to a study by the Kaiser Foundation. Most family doctors make less than half that.
The search for solutions
Any healthcare professional in New York City will tell you that something has to change. For one thing, the city has to attract more doctors to practice in its poorer precincts. The city’s Health and Hospitals Corporation recently announced $11 million in scholarships for city residents who attend St. George’s University Medical School, in the Caribbean nation of Grenada, and agree to return to practice as primary-care physicians in the city’s public health system.
That’s only one effort to improve city health services. In addition, a mentoring program is encouraging local medical students to consider a career in family medicine.
Many analysts say the bottom line must be more money. Primary care will have to pay more to entice a new generation of doctors.
Another experiment attempts to reduce the unnecessary use of ambulances. Reformers hope to create a system of “community paramedics,” who would visit the frequent fliers and encourage them to seek better overall healthcare.
Clinics are testing a model of care called the “patient-centered medical home,” which advocates say provides better outcomes at lower costs by taking better care of patients and keeping them out of the hospital.
At Montefiore Medical Center, in the Bronx, Medicare is sponsoring a similar experiment in collaboration, known as an Accountable Care Organization. If successful, the approach could spread across the country.
All of these initiatives may be part of the solution to the primary-care crisis. Many analysts say the bottom line must be more money. Primary care will have to pay more to entice a new generation of doctors.
Various proposals are circulating. The American Academy of Family Physicians calls for increased federal funding for medical-school departments of family medicine, increased payments to family physicians for clinical services, and insurance reforms that lead to higher payments for primary-care services.
Beyond questions of pay, primary-care providers will remain a special kind of doctor. The best of them communicate easily with their patients, don’t mind working long hours, and have the sense and creativity it takes to make good diagnoses.
Norah Garry, 28, a student at the SUNY Downstate College of Medicine, sought advice from an experienced pediatrician as she debated whether to go into primary care.
Go for it, the older doctor advised.
What about all her student debt? Garry asked her. “‘I had those same loans and I made it work,’” Garry recalled her mentor telling her. “She said, ‘Base your decision on what makes you happy, not how much money you’ll make.’”
Garry took the plunge, and is now a resident at Children’s Hospital Montefiore, serving some of the toughest neighborhoods in the Bronx.
Her case gives hope that other young doctors can be persuaded to follow her into the healthcare desertlands. It suggests that one day the benefits of decent healthcare will stop withering, and start blooming throughout New York City.
Leave a Reply
You must be logged in to post a comment.

3 Comments
David Lewis
May 23, 2012Fascinating and troubling that the most basic needs are the least valued. Especially when you consider that in the Bronx, for instance, the health-care industry is the largest employer in the borough. Good work bringing this to light!
Molly Sweeney
May 27, 2012As a former volunteer and later recruiter for Doctors Without Borders, I know for certain there are many, many doctors out there who are sick and tired of the the “big business” of medicine and the wretched constraints of “big profit” insurance companies. I listened to their tales of despair over and over again. Some of them sought our organization as a way of making their way back to why they originally wanted to become doctors. Some were dreading the prospect of jumping into the system and were looking for a way to manage their debt while following their hearts.
The solutions are there – and you outline them well. For heaven’s sake channel some health care dollars into subsidizing the medical school costs for those who commit to going into family practice. The health benefit of providing primary care and preventive services to our communities will more than make up the obscene costs of walking into an ER to get ear aches and colds treated. The population wanting to do this work will be there.
And, of course, pay those doctors decently by sucking some of the over-the-top profits from our big Wall Street stars: pharmaceutical and insurance companies. It’s ridiculous what a heart surgeon makes in comparison to the guys in the trenches are reimbursed. Just who is deciding who gets paid what? And who’s given them that power???
These issues are manageable. The real question is whether blathering politicians will so obscure the issues in bipartisan rhetoric that they will never have the opportunity to be addressed.
Eric Keahey
January 30, 2014The problem centers around the fact that CMS has a board which controls medicare funding and decides how much is paid for what service. This board is composed of primarily specialists, I believe 18-20 specialists, a handful of non-medical ‘experts’ in the field, and 1-2 primary care docs. This board decides how much medicare pays for everything from a basic physical with your family practice doctor, to how much is paid for getting your gallbladder taken out. Private insurance rates are typically a factor of the Medicare rate, ie 110% of Medicare, 140% of Medicare, etc, so this board is tremendously powerful in Healthcare finance.
When faced with cutting medical costs, guess where a board composed of mainly specialists takes money from? They cut rates for primary care, and pad their own pockets. This has been the system for DECADES, and is one of the main reasons our healthcare system is failing us. A primary care doc needs to see 25+ patients per day to stay afloat because of this, which is why you feel rushed when you see them. In contrast, a gastroenterologist does a 20 minute colonoscopy, and gets paid several thousand dollars for it.
Other countries, primarily in Europe, where primary care is valued, have better primary care physician satisfaction, better overall costs for healthcare, and BETTER PATIENT OUTCOMES. Yes, more specialists, in many studies, have been shown to make you more likely to have complications, cost more, and can even increase your risk of death. Good primary care is the foundation of an effective medical system. Our foundation is faltering.
If you haven’t guessed already, I’m a family practice doc. I may be biased, but I can quote studies for most of what I mention here.